If I Get to Sixty Four
There is some surprising news going around about middle-aged white Americans and it has nothing to do about presidential politics and Donald Trump. Two Princeton economists published a report showing that the “all-cause” mortality rate for middle-aged whites (men and women) has dramatically increased between 1999 and 2013. This increase was largely driven by increased death rates from drug and alcohol poisonings, suicide, chronic live diseases and cirrhosis. While all education groups saw increases in mortality from suicide and poisonings, individuals with lower amounts of education had the most marked increases.
Self-reported declines in health, mental health, and ability to conduct activities of daily living, and increases in chronic pain and inability to work, as well as clinically measured deteriorations in liver function, all point to growing distress in this population.
Several news outlets have commented on this startling report, including The New York Times and NPR. Just a thought: I wonder how many of the reporters are white middle-aged Americans.
The Princeton economists are husband and wife: Dr. Angus Deaton and Dr. Anne Case. Deaton just won the 2015 Nobel Prize in Economics. They said they stumbled on their finding by accident. They were looking at health and mortality data from the Centers for Disease Control and Prevention (CDC) and other sources that asked people about their levels of pain, disability and general ill health. Deaton was looking at statistics on suicide and happiness. Case was investigating poor health, including chronic pain. She herself has suffered from chronic disabling lower back pain for 12 years.
Dr. Deaton noticed the high rates of suicide for middle-aged whites in national data sets, and that the all-cause mortality in this group was rising. He and Dr. Case realized suicides alone would not be enough to push up the overall death rates, so they began to look at other causes of death. “That led them to the discovery that deaths from drug and alcohol poisoning also increased in this group.” NPR quoted Deaton as saying: “Pretty quickly, we started falling off of our chairs because of what we found.”
There was this extraordinary turnaround, which is sort of something like – you would say the ship’s been going in this direction for a very long time, and then all of a sudden, it just reverses and goes the other way. And when we saw this, that was the thing that sort of really thought, oh, my goodness, we have something here that we really haven’t seen before.
In their report, Case and Deaton said this increased mortality is only partly understood. Increased availability of opioid painkillers began in the late 1990s. The tighter control on opioid prescriptions could have led to some substituting heroin. At the same time there was increased availability, falling prices and better quality with heroin. However, the prevalence of pain, which the opioids were ostensibly to treat, can’t be pointed to as either a cause or an effect for the increase of opioid use. “Both increased rapidly after the mid-1990s.”
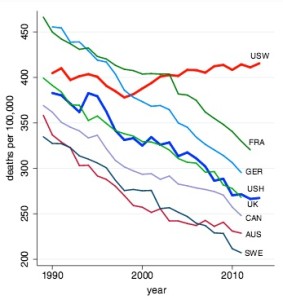
Speaking to NPR, Deaton noted how declining mortality statistics were typically viewed as one of those that indicated how well a nation was doing. The following figure, taken from the Case-Deaton report, shows a reversal of the decline in midlife mortality for US whites after 1998. Before that time, the mortality rate had been falling by 2% per year on average. After 1998, while other countries’ mortality rates continued to decline, US rates started to rise. No other country had a similar turnaround.
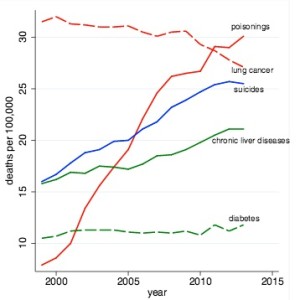
 They also looked at causes of death and found that three causes of death accounted for the reversal in mortality rates, namely suicide, drug and alcohol poisoning (accidental or intentional), and chronic liver diseases and cirrhosis. All three rose yearly after 1998. For comparison, they added mortality rates for lung cancer and diabetes. Notice how suicides are trending to surpass lung cancer as a cause of death in the near future. “Poisonings overtook lung cancer as a cause of death in 2011.” See the following figure, also taken from the Case-Deaton report.
They also looked at causes of death and found that three causes of death accounted for the reversal in mortality rates, namely suicide, drug and alcohol poisoning (accidental or intentional), and chronic liver diseases and cirrhosis. All three rose yearly after 1998. For comparison, they added mortality rates for lung cancer and diabetes. Notice how suicides are trending to surpass lung cancer as a cause of death in the near future. “Poisonings overtook lung cancer as a cause of death in 2011.” See the following figure, also taken from the Case-Deaton report.
 Case and Deaton suggested their findings could help explain recent large increases in Americans on disability. In conclusion, they expressed concern that those now in midlife could age into Medicare with worse health issues than the current elderly. This won’t be automatic, especially if the noted trends are brought under control. “However, addictions are hard to treat … so those currently in midlife may be a ‘lost generation’ whose future is less bright than those who preceded it.”
Case and Deaton suggested their findings could help explain recent large increases in Americans on disability. In conclusion, they expressed concern that those now in midlife could age into Medicare with worse health issues than the current elderly. This won’t be automatic, especially if the noted trends are brought under control. “However, addictions are hard to treat … so those currently in midlife may be a ‘lost generation’ whose future is less bright than those who preceded it.”
Ronald Lee, a professor of economics and demography and the director of the Center on Economics and Demography of Aging at the University of California, Berkley said: “Seldom have I felt as affected by a paper. It seems so sad.”
It seems quite apropos to whimsically close this article by listening to the Beatles song, “When I’m Sixty Four.” And who better to sing it given the above commentary than The Apollo Club, an all-white, mostly middle-aged choir.

